Andrea N. Polonijo, a Chancellor's Postdoctoral Fellow in the Department of Social Medicine, Population, and Public Health at the UCR School of Medicine, is a coauthor on a study, “Social Determinants of Shingles Vaccination in the United States,” that examines how sociodemographic characteristics, health behaviors, and self-rated health are associated with shingles vaccine uptake.
Published in the Journal of Gerontology: Social Sciences, the study is led by Eric M. Vogelsang at California State University–San Bernardino.
Polonijo explains the findings of the study in this Q&A:
Q: You found that “Black and Hispanic older adults have almost 50% lower odds of shingles vaccination compared to Whites.” What are the reasons for this?
This is likely explained by some of the same factors driving racial-ethnic disparities in flu vaccination, such as: limited healthcare access, lower levels of vaccine awareness, lower likelihoods of receiving provider recommendations to vaccinate, greater concerns about vaccine safety, greater rates of medial mistrust, and language barriers.
Q: How are sociodemographic characteristics and health behaviors associated with shingles vaccine uptake?
Women are more likely to get vaccinated against shingles than men, which may be related to them seeking more preventive health services overall. People with higher levels of income and education are also more likely to be vaccinated, which is likely due in part to differences in knowledge and insurance coverage. Geographically, the U.S. territories and East South Central states have the lowest rates of shingles vaccination, warranting further attention.
People who engage in healthy behaviors — including not smoking, exercising and eating vegetables regularly, wearing seatbelts, and getting yearly health checkups and flu shots — are more likely to be vaccinated than to people who don’t. Given two of these health behaviors (yearly health checkups and flu shots) are tied to healthcare services, health providers likely have an important role to play in promoting shingles vaccine uptake through recommendations. Administering flu and shingles vaccinations together, in a single doctor’s office or pharmacy visit, may also help to encourage uptake and is considered safe.
Q: You also report that “abstaining from alcohol, being employed, living with children, and having poor self-rated health are also associated with lower uptake. Unmarried (vs. married) individuals have lower odds of vaccination that are explained by broad differences in health behavior.” How might this be explained?
It could be that some people who abstain from alcohol also forego shingles vaccination because they feel both are “foreign substances” that could negatively impact their health. Older adults who are employed or living with children may have greater time constraints that prevent them from getting vaccinated. The shingles Zostavax vaccine was not recommended for those with “weakened immune systems,” which might have led some older adults who felt their health was poor to cautiously avoid it. People who are married tend to engage in more healthy behaviors overall, likely because their spouses encourage healthier habits.
Q: Finally, what are the other findings reported in the paper?
We found only about 35% of older adults have been vaccinated against shingles. Though rarely fatal, shingles can lead to long-term neuropathic pain, brain inflammation, and other severe long-term complications that are preventable with vaccination. At a time when there is increased politicization of vaccines and viruses, our study is a step towards understanding why many of U.S. older adults have yet to be vaccinated.
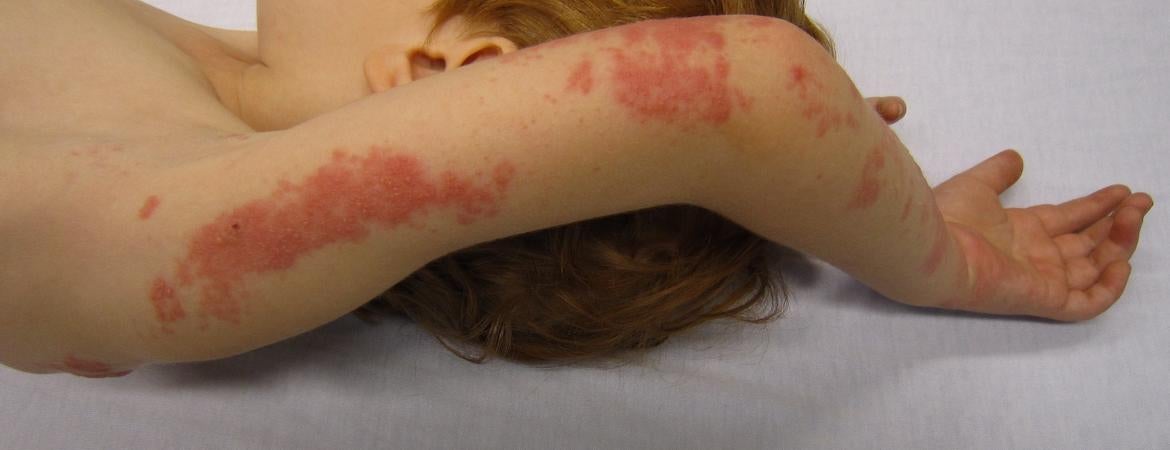
Header/thumbnail photo: A child with shingles by James Heilman, MD, on Wikimedia Commons